Cow's Milk Protein Allergy (CMPA) and Your Baby
This article is a BIG one addressing all things cow's milk protein allergy (CMPA) and your baby!

This article is a BIG one addressing all things cow's milk protein allergy (CMPA) and your baby! Buckle up because it gets a little bit into good ol' chemistry.
And as always, nothing in this blog article is meant to replace medical advice from your healthcare provider.
Jump to:
First, what is a CMPA?
CMPA is short for cow's milk protein allergy. This is when the body reacts to the specific protein in cow's milk. The immune system responds abnormally to cow's milk and can result in unpleasant and potentially life-threatening allergic reactions. Unfortunately, CMPA is one of the most common food allergies in babies. Many children outgrow it by age 1 to 3. However, a small percentage will not.
It's difficult to find reliable stats, but about 3 - 7 babies out of 100 will develop CMPA. This is just a reflection about the tricky nuances of data collection! Oh science!
What are the signs/symptoms of CMPA?
These are the most common physical signs that a baby may have a CMPA:
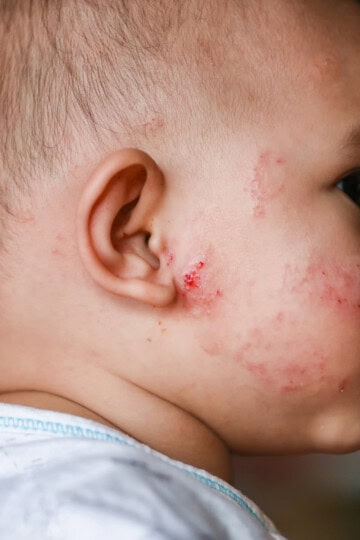
- rashes, eczema, hives, swelling of face and lips
- stomach and gut problems like nausea, vomiting, diarrhea, stomach pain, blood or mucus in stools
- airway problems like a runny nose, wheezing; troubled breathing, drooling, gagging
- baby is not gaining weight as expected
How is CMPA diagnosed?
It's important to get a firm diagnosis of CMPA by working with your healthcare practitioner. We realize resources will vary from community to community but this is a big part of your child's health history. It's also an opportunity for providers to rule out other diseases.
Your provider may use a variety of ways to help with diagnosis such as an elimination diet followed by a challenge, skin prick test, patch test or a blood test. However, the elimination diet followed by a challenge is the "gold standard".
Difference Between CMPA and Lactose Intolerance
Before we dive in, it's important to note: breastmilk is FULL of lactose, It's the principal sugar in human milk…this means, infants were *meant* to tolerate it.
There is some definite confusion among parents around identifying if a baby has lactose intolerance vs CMPA, but the two are very different. If you need support diagnosing this, it's best to work with your health care practitioner.
When we think about a dairy allergy, we're talking about the PROTEIN in milk.
When we think about a lactose intolerance, we're talking about the SUGAR in milk.
In all honesty, lactose intolerance among infants is very rare. Like…super-duper rare. If a baby presents with congenital lactose intolerance they typically present with severe diarrhea, vomiting, dehydration and poor growth. We also see these symptoms in babies with a rare disorder known as galactosemia. In these cases, a medical team would be helping and a soy based formula would be offered. Typically, parents cannot breastfeed baby. Breastmilk contains lactose regardless of whether the nursing parent consumes it. Congenital lactose intolerance and galactosemia would most likely be evident shortly after birth.
In our research, we've also learned that some pre-term babies may have a temporary lactose intolerance simply because their body isn't producing lactase enzymes just yet (this is the enzyme needed to breakdown lactose, the sugar in milk)! But don't worry, if you're hoping to nurse you can continue to offer your human milk and babe's enzymes will start to kick in. If you're a formula feeding family, your babe may benefit from a low lactose or lactose free formula, and eventually you can look at transitioning off.
What about your older child?
From the data we've reviewed, it appears as though lactose intolerance is very rare in children under 5 years of age! Phew! If you suspect your child is intolerant to lactose, work with a Registered Dietitian to help. Your child can likely still tolerate many forms of dairy that contain lower levels of lactose or lactose free products.
What To Do if CMPA is Suspected?
Okay, you've noticed signs and symptoms that your baby may have a CMPA and you've visited your healthcare provider for an assessment. Now what? This information might be particularly helpful if you haven't quite started solids yet!
PLEASE NOTE: don't go at this alone. Restricting any diet unnecessarily is never the goal; discuss with your Dietitian or health care provider! Also...this does not replace medical advice you've received.
Step 1:
Nursing or Breastfed Baby: nursing parent needs to remove all dairy (including trace amounts) from their diet and may benefit from a calcium/vitamin D supplements.
Formula Fed Baby: switch to an extensively hydrolyzed casein formula. In some cases, your healthcare provider may even suggest an amino acid based formula.
Step 2:
Stick with the new plan for 72 hours. If cow's milk was the culprit, then symptoms should start to ease up at this time, although full resolution may not be seen for up to two weeks.
Step 3:
If symptoms have started to resolve, continue with the dairy-free/extensively hydrolyzed plan. If symptoms have not started to resolve, consult your baby's pediatrician!
Step 4:
If symptoms resolve, double confirmation that cow's milk was the culprit is an important part of the picture. The nursing parent should resume a dairy containing diet or the formula fed child should resume standard formula. If symptoms reappear, then it's confirmed! Again, this challenge is an important piece and can be overlooked.
Step 5:
If symptoms reappear with the dairy challenge then go back to dairy-free plan!
Extensively hydrolyzed formula is expensive and sticking with a dairy-free diet can be challenging so it's important not to impose these restrictions on a family, if they're not necessary!
How Long Does it Take for Milk Proteins to Clear Breastmilk?
Have you heard that it can take 2-6 weeks for cow's milk to be removed from a nursing parent's system after cutting it out?
Thankfully this just isn't true!
Just imagine how heartbreaking and guilt-inducing it would be if a breastfeeding mama accidentally ate some dairy! To think that she might be subjecting her child to symptoms for the next couple of weeks simply because she thought the pesto she ate was dairy-free when it actually wasn't.
In fact, dairy protein fragments are cleared from mother's milk 6 HOURS after ingesting them. How cool is that?
This is sooo important to know because some women will decide to wean from the breast out of caution for their child (not because they wanted to wean) when it wasn't actually necessary!

How to Introduce Solid Food to a Baby with CMPA
If your baby has a cow's milk protein allergy (CMPA), the good news is that there's very limited impact when they initially start solids… for the first few months, at least!
For all babies, we recommend initially avoiding serving large amounts of dairy (a sip of your smoothie here and there or using some yogurt in muffins is fine) as it can interfere with iron absorption, which is the top nutrient to focus on at that age!
So for those babies with CMPA, you'll just need to continue to avoid even small or tiny exposures to dairy. Watch out for iron-fortified infant cereals too. You'll want to choose one that says "add breastmilk or formula" in the preparation instructions. The "add water" types contain skim milk powder which would not be safe for a baby with CMPA.
You'll also want to pay particular attention when introducing the other top allergens as babies with CMPA are at a higher risk of being allergic to other foods. But, unless you were specifically directed otherwise, there's no need to DELAY introducing those allergenic foods like peanuts and eggs.
The story changes closer to 12 months when your baby's needs for calcium nearly triple!
Thankfully many babies with CMPA outgrow the allergy by this age.
If your baby is on an extensively hydrolyzed formula, it contains slightly less calcium than whole cow's milk. Including some high calcium non-dairy food options in baby's diet will help to meet his needs (see below for ideas!).
But if your baby is breastfed, you'll want to strategically include plenty of high calcium non-dairy food options to your own diet as human milk contains roughly ⅓ the calcium as cow's milk.
When And How to Re-Introduce Dairy to a Baby with CMPA
About 80% of babies will outgrow their milk allergy by age three! Doesn't that statistic fill you with so much hope?
So, how do you know if your baby has outgrown their milk allergy? The only way to know (unfortunately), is to feed your baby dairy and check for a reaction!
We know that can be a scary thought! And BIG DISCLAIMER here: please do not attempt to re-introduce dairy without the guidance of your baby's healthcare provider. They will assess whether it's safe for your baby or whether you should wait longer.
But what makes it less scary, is that you'll follow a slow-paced, step-by-step plan called the milk ladder.
The milk ladder is a step-by-step plan to introduce dairy first in its least allergenic form and slowly moving up to its most allergenic form. There are a variety of different plans; some have 4 steps while others have 12 steps. Your healthcare provider will set you up with the one that is best for your baby.
Pictured here is an example of a six step plan:
- Step 1: baked biscuit
- Step 2: muffin
- Step 3: stovetop cooked pancake
- Step 4: cheese
- Step 5: yogurt
- Step 6: fluid milk

Once your baby passes one step, after a set amount of time (as determined by your baby's healthcare provider), you will graduate your baby to the next step until eventually they may be able to tolerate fluid milk!
Sources:
https://www.albertahealthservices.ca/assets/info/nutrition/if-nfs-milk-allergy-birth-to-3-years.pdf
https://pubmed.ncbi.nlm.nih.gov/392766/
More Articles Your Family Will Love
Should I Buy Organic Food For My Baby?
How to Feed Your Baby According to Their Personality
How Farmers are Keeping Food Costs Lower for Your Family
What no one talks about: Everything You Need to Know About Formula




Very informative, we are currently in the elimination process with my 6 month old. It's been a challenge eliminating dairy in my diet.
Yes, dairy can be "hidden" in a lot of foods. Best wishes to you as you navigate this elimination process.
All the best with the elimination process and the overall journey to 'conquer' your baby's allergy. Remember that soy, beef and egg have the same protein 'built up' as dairy, our specialist doctor advised me to eliminate them all at the same time. It was a huge change in our little one's whole health being, albeit a tough one for me. There are many support groups on Facebook that have the best tips for food recipes and other advise. All the best.
Hi, you said that there’s links below for high calcium recipes that don’t include dairy but I don’t see them! Can you please link? Thanks!
Hi Livia,
Thanks for catching that. I've linked it now but here's the article we have on high calcium foods for the dairy free baby: https://happyhealthyeaters.com/calcium-for-your-dairy-free-baby/